What Is Food Intolerance
On this page
Introduction
Food Intolerance is an abnormal reaction to food 1 that occurs inside and outside of the digestive system.
More than 20% of the population in industrialized countries suffer from food-related unpleasant reactions, and these reactions are on the rise. Those foods our bodies do not agree with can cause serious damage! We need to note that the majority of cases of adverse reactions to food (15% to 20%) are due to non-immunological causes and only 2-5% of cases of in adults and 10% in children are caused by the “true” allergy. In the scope of this article, we cannot identify all root causes, but the numbers are frightening. Dalhousie University report 2 confirms that about 10% of Canadians have food allergies, and about 20% suffer from a food intolerance!
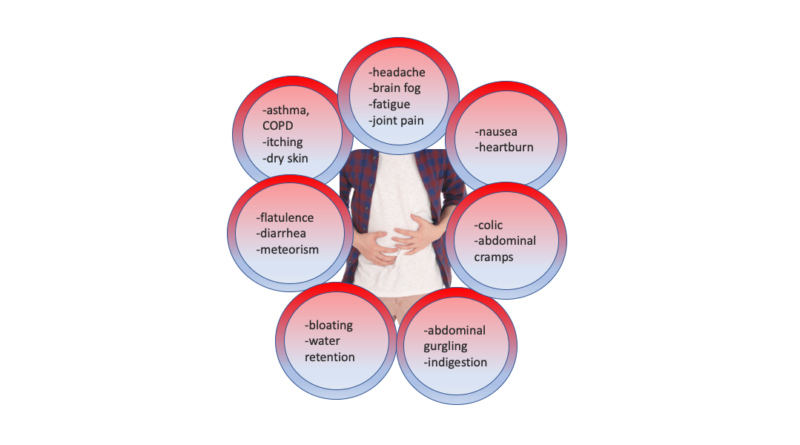
The wide range of reactions includes some pseudo-allergic effects 3:
- headache
- brain fog
- asthma
- heartburn
- indigestion
- colic and abdominal cramps
- diarrhea
- flatulence
- bloating and abdominal gurgling
- meteorism
- nausea
- itching and dry skin
- water retention
These effects can be caused by:
- salicylates, biogenic amines (such as histamine, tyramine, serotonin etc.),
- sulfites (present in wine and medications),
- sodium glutamate (flavor enhancer),
- colorants and preservatives (such as tartrazine, benzoates, sorbates etc.),
- sweeteners (aspartame),
- lack of enzymes.
When we are talking about Food Intolerance, we agree to address only special responses that do not involve immune system. In other words, IgE/IgG immunoglobulins do not modulate reactions that we attribute to Food Intolerance 4, and corresponding tests, though very useful to identify allergy type 2 reactions, cannot be used to identify foodstuffs causing responses not modulated by the immune system.
Classification of Adverse Reactions to Food by Pathophysiology
All adverse reactions to foods can be classified according to their underlying pathophysiology as the following 5:
- Toxic (ingested food toxins, rather infrequent): i.e. scombroid syndrome from the ingestion of spoiled fish containing a lot of histidine which is transformed into histamine in the gut by bacteria.
- Non-toxic
Immune-mediated (food allergy)
Reaction to foreign protein accompanied by release of allergy mediators
- IgE-mediated immediate reactions
- non-IgE (i.e. IgG, IgA, IgM, cell, or immune complexes) mediated delayed reactions
Non-immune mediated (food intolerance)
- Enzymatic, resulting from enzymatic defects of the gastrointestinal tract i.e. lactose or gluten intolerance
- Pharmacological, caused by vasoactive amines (dopamine, histamine, norepinephrine, phenylethylamine, serotonin and tyramine) and other substances present in foods, all of which manifest pharmacological activity. In most cases, there is a dose-effect relationship. I.e. foods which contain high quantities of histamine may provoke symptoms similar to those of an allergic reaction, but normally, histamine is rapidly inactivated by enzyme di-aminoxidase (DAO) in the gastroenteric tract.
- Undefined, resulting from non-identified mechanisms, such as food additive reactions. Those who is predisposed may show intolerance reactions to sulphites, nitrites, nitrates, monosodium glutamate and some colourings. Possible symptoms are asthma, rhinitis, urticaria, itchiness, and migraines.

Classification of Adverse Food Reactions by Reaction Type
Food Intolerance reactions can be classified into metabolic reactions, anaphylactoid reactions, and idiosyncratic reactions6, 7.
Metabolic Reactions
These are adverse reactions that result from a defect in the body’s ability to metabolize certain food components. An example of this is an intolerance to cheeses and milk (enzymatic pathophysiology). Symptoms of dairy products intolerance include abdominal cramping, bloating, and flatulence.
Adverse reactions to consumption of dairy products may root in lactose intolerance resulting from a deficiency of the enzyme lactase. As a result, lactose cannot be metabolized and absorbed by the small intestine. Then, lactose passes into the colon, where bacteria metabolize it into carbon dioxide and water causing indigestion symptoms. Some foods just can have a negative impact on the metabolic system 8 manifesting in a variety of ways, due to a systemic incompatibility.
Please note that other components of the foodstuff, such as pesticides, colourings, or excessive bacterial load, also may be responsible for intolerance reactions.
Anaphylactoid Reactions
Result from the ingestion of substances that are high on histamine 9 and/or trigger release of histamine from cells within the body (pharmacological pathophysiology type).
These reactions also do not involve the IgE-mediated response. An example of this type of reaction is the strawberry reaction because it contains very little protein, no allergies have been identified, and there is no evidence of a strawberry-specific IgE. Nevertheless, strawberries have been known to cause allergy-like symptoms. Therefore, an anaphylactoid reaction is a logical explanation.
Large doses of ingested histamine from cheese or spoiled fish can overwhelm the body’s ability to metabolize it, especially in those with histamine intolerance due to mast cell activation disorders and reduced ability to metabolize histamine. The excess histamine is absorbed, enters the bloodstream, and causes symptoms very similar to food allergies (but not allergies!).
To prevent complications from excess histamine, you need to reduce the amount of histamine circulating in your body. The article “Histamine Intolerance: Am I Crazy or Allergic?” explains how excessive histamine (aka “histamine intolerance”) could bring havoc to your body.
Idiosyncratic Reactions
Idiosyncratic reactions involve adverse reactions that occur in individuals via an undefined pathophysiological mechanism. The best example of this type of reaction is the sulfite-induced asthma. Although the mechanism of this reaction is unknown, the relationship of the food to the reaction has been well documented. Asthma is the most common symptom involved, following ingestion of sulfite.
Addressing Food Intolerance in Disease Management
Managing adverse food reactions is a significant part of the chronic disease control, especially lung disease. It consists of managing the immune and non-immune factors.
To maintain quality of life and avoid disease exacerbations, allergy medications along with food avoidance are recommended 10.
You may want to start by reducing the amount of histamine your body releases. Substances calming down your cells histamine release are called mast cell stabilizers. Quercetin is a substance whose stabilizing function is at par or even better than prescription medications 11. Seeking Health provides trusted, made-in-the-USA, and properly tested supplements, including Gut Nutrients blend with Quercetin.
You continue by improving your ability to metabolize released histamine. DAO (Diamine Oxidase) in your gut is responsible for histamine metabolizing. Seeking Health offers THE BEST on the market DAO supplement, for you to able to eat and drink again! To get these supplements, just click on the images below and use code IQ10 for 10% discount at checkout.
In general, measures to avoid food culprits result in considerable improvement in disease symptoms (i.e. asthma), reduction in drug therapy, and hospital admissions.
The problem is how to reliably identify these offensive foods, with high degree repeatability, and figure out minimal avoidance period to prevent intolerances (and thus disease exacerbations, i.e. in asthma and COPD) from reoccurrence. Non-immune mediated food intolerance reactions (sometimes called metabolic) are more volatile and are more tricky to identify. This is a significant area of the disease management which more often than not is going unattended.
So far, only about 25% of all identified Food Intolerance cases are addressed by the alternative health care practitioners, such as nutritionists. In our opinion, successful restoration of life quality requires efforts from all involved parties, and nutritionists play deciding part in it. But this may be a long, quite expensive, and tedious process that requires joint, synergetic effort from you and your health support team:
- with the help of your general practitioner, you need to identify underlying conditions, such as mast cell activation disorder, liver abnormalities, IBS or structural problems – and address them accordingly
- your allergist will help to find “true” allergies and delayed hypersensitivities through IgE/IgG tests, skin patch testing etc to identify foods which need to be excluded, likely indefinitely
- your psychologist will help you to clean up psychological climate in your life, so you can identify and control factors affecting severity of exacerbations
- your nutritionist will follow with you on elimination diet to identify Food Sensitivities and temporary exclude and re-introduce the foods (that may be the least pleasant for you and the lengthiest part)
- your nutritionist will also help with assessment of your environment and deal with nutritional deficiencies
This process may take months, if not years, and cost thousands of dollars. Even worse, your body can incur irreparable damage, especially when you self-diagnose or self-medicate. So, is there a light in the end of the tunnel? Is it possible to go back to normal and predictably control your food response symptoms? The definite answer is: YES!
But is Food Intolerance a disease to control?
No, it is not! As it is defined by Daphne Lab’s®, Food Intolerance is not a disease, and there is no pill against it, but there are solutions. This problem may be and needs to be controlled.
We can help with the lengthiest and the most unpleasant part, the identification of offensive foods and substances and the frequency of their consumption. Then, by giving your body a rest and changing the frequency of ingestion, you are given a chance to step on the road to recovery, wellness, and improved life quality!
We administer and follow up the North American-tailored version of Daphne LabⓇ BioMetaTests (Italy) that is exclusively available through Montreal-based company Fresh Start Testing™. One test assesses your body’s sensitivity to 1,100+ foods, including about 300 North American/Canadian food items! Daphne LabⓇ BioMetaTests:

- satisfy needs of 90,000+ clients annually, in more than 80 countries
- are used in Italian hospitals
- are ISO-compliant
- utilize patented bio-spectrophotometry methodology
- have 94% repeatability and reliability rate
- are administered only through trained professionals
References
- Plant & Soil Sciences Library. Lesson: Non-Immunological Reactions. Downloaded on April 6, 2022
- Dalhousie University – Agri-Food Analytics Lab Report Downloaded on April 11, 2022
- Zopf, Y., Baenkler, H. W., Silbermann, A., Hahn, E. G., & Raithel, M. (2009). The differential diagnosis of food intolerance. Deutsches Arzteblatt international, 106(21), 359–370
- Mohamed H. Shamji, Rudolf Valenta, Theodore Jardetzky, Valerie Verhasselt, Stephen R. Durham, Peter A. Würtzen, R.J. Joost van Neerven. The role of allergen-specific IgE, IgG and IgA in allergic disease. Allergy, 10.1111/all.14908, 76, 12, (3627-3641), (2021).
- Claudio Ortolani, Elide A. Pastorello, Food allergies and food intolerances, Best Practice & Research Clinical Gastroenterology, Volume 20, Issue 3, 2006, Pages 467-483, https://doi.org/10.1016/j.bpg.2005.11.010.
- Lemke PJ, Taylor SL. Allergic reactions and food intolerances. In ‘Nutritional Toxicology,’ ed. FN Kotsonis, M Macke, J Hjelle, pp. 117-137.
- Metcalfe DD. Food hypersensitivity. J. Allergy Clin Immunol. 1984a. 63; 749-762.
- The FOOD INTOLERANCES: a path of knowledge. From Daphne Lab’s®. Downloaded on April 6, 2022
- Kovacova-Hanuskova E, Buday T, Gavliakova S, Plevkova J. Histamine, histamine intoxication and intolerance. Allergol Immunopathol (Madr). 2015 Sep-Oct;43(5):498-506.
- Isobel Stoodley, Lily Williams, Cherry Thompson, Hayley Scott, Lisa Wood Evidence for lifestyle interventions in asthma Breathe 2019 15: e50-e61; DOI: 10.1183/20734735.0019-2019
- Mlcek, J.; Jurikova, T.; Skrovankova, S.; Sochor, J. Quercetin and Its Anti-Allergic Immune Response. Molecules 2016, 21, 623. https://doi.org/10.3390/molecules21050623